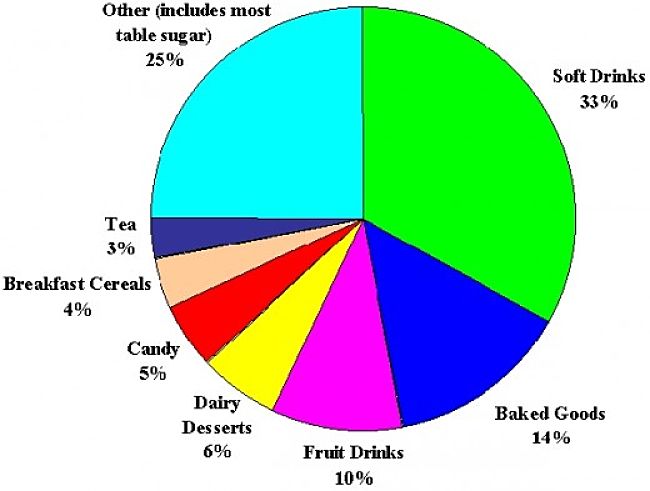
Low Carb Sugar Cravings & Natural Ways to Stop Sugar Cravings
There has been a lot of debate about whether refined sugar and corn syrup could be the addictive trigger for food cravings that ruin most diets, especially low-carb diet plans. Most diets fail, and most people that lose some weight on diets, put it all back on eventually.
Recent research has suggested that processed and refined sugar (sucrose) and corn syrup could be linked to an addiction-like experience in the brain. These addition-like responses resemble the addition to coffee, nicotine and to many drugs.
Can we become addicted to sugar or corn syrup so that the crash in blood sugar levels triggers a need for a new sugar hit?
Is this the reason why dieters develop sugar cravings that are very hard to control?
This article reviews the research about whether sugar cravings are caused by an addition to sugar and the quest for a natural remedies to sugar cravings.

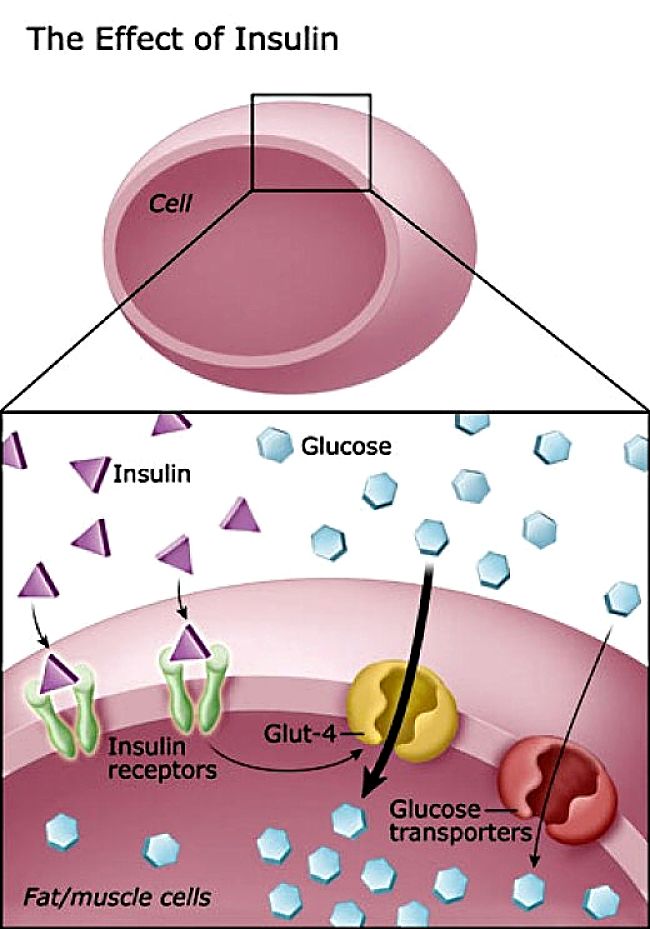
Normal Metabolism of Glucose and the Role of Insulin
Most food you eat will be digested and metabolised to fatty acids, amino acids and the simplest sugar molecule - glucose. This sugar in the form of glucose then enters the bloodstream from which it is picked up by the various cells in the body as a form of energy or fuel to drive all the metabolic processes in the body. The hormone insulin, produced by the pancreas, plays a major role in this process. As shown in the image above, the insulin acts as a trigger or facilitator to allow glucose from the bloodstream to enter the cells of the body. Insulin is released naturally to maintain the level of glucose in the blood after eating and between meals.
After a meal the glucose level in the blood rises and this triggers the release of insulin so the glucose can flow into the cells. This lowers the blood glucose level. The excess glucose in the blood can be absorbed into the liver and muscles and converted to glycogen. Some glucose can also be converted to fatty acids and stored in fat cells. This process is reversible so that glycogen, or even fat or protein, can be used as an energy store and converted back to glucose between meals to maintain blood glucose levels. In a sense the blood glucose is like the fuel in the fuel line of a car, with insulin acting as a fuel injector or carburettor to meet the demands of the engine for more or less power and speed.
If the insulin response does not occur the normal glucose metabolism will not work properly. This leads to the condition of diabetes which can be regarded as insulin resistance. When there is insufficient insulin released or the body’s response to insulin is blocked or diminished blood glucose levels can rise well above the normal level.
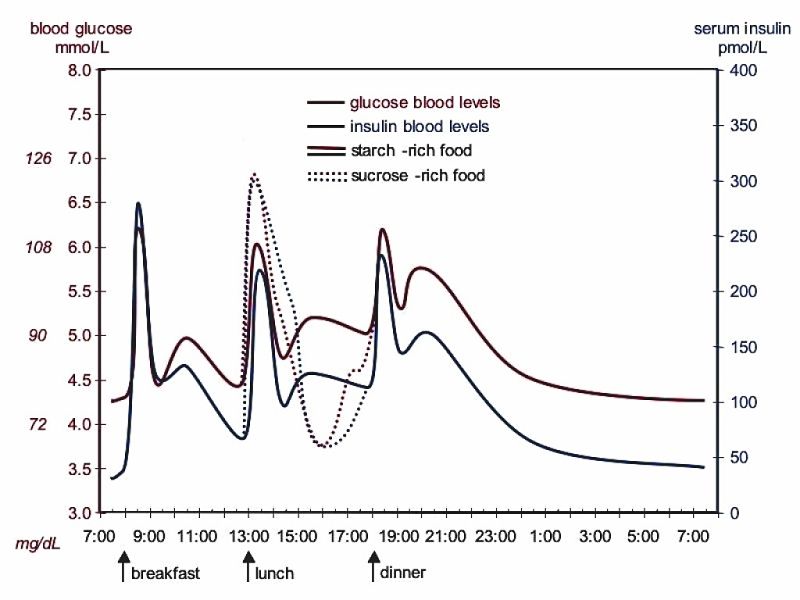
Blood sugar levels normally rise and fall before and after eating, and there is an accompanying rise and fall in insulin levels. Eating sugar tends to produce a very pronounced rise and fall in blood sugar compared with eating whole foods. This is shown in the image below.
How Does the Glycemic Index and Glycemic Load Effect Blood Sugar Patterns After Eating Foods?
GI or the glycemic index (glyceemic index)
This provides a method for estimating of how quickly the levels of glucose in the blood are expected to rise after consuming different of type of food. Pure Glucose has a glycemic index of 100 and foods are normally given a GI value as a percent age relative to pure glucose. The glycemic index is essentially a measure of the amount of readily available carbohydrate in the food.
GL or the glycemic load (GL) of food
This is essentially the load of carbohydrate in the food expressed as the glucose raising effect of the food in amounts equivalent to consuming 1g of pure glucose.The Glycemic load takes into account the amount of carbohydrate in the food consumed. For example, melon is generally regarded as a high GI food because the carbs it contains are readily available, but melon is a food with low calorie density as it is mostly fiver and water. A standard serving of melon such as 100g has much less carbohydrate than yogurt for example. So the Glycemic Load of melon is low. The glycemic index is generally used for a single ingredient or individual type of food. On the other hand, the glycemic load can be calculated for any portion or serving of food, for a mixed food dish or entire meal, or all the food consumed during a day.
For a standard serving of a food:
- a GL greater than 20 is considered high and these foods mostly have low GI ingredients
- a GL of 11-19 is considered medium,
- a GL of 10 or less is considered low and these foods most have high GI ingredients
Foods that have a low GL for a standard serving size generally have a low GI.
How Does GL and GI Affect Blood Glucose Spikes and Create Sugar Cravings?
Various research studies have examined how the amount of sugar eaten affects the blood sugar cycle and the hunger response. One recent studies examined how the Glycemic Index and Glycemic Load of food eaten affected the pattern of blood sugar levels after a meal.
Overweight women were given one of four meals in random order:
- Low portion meals with a low glycemic index (40–43%)
- Large portion meals with a low glycemic index (40–43%)
- Low portion meals with a a high-glycemic index (86–91%)
Blood samples were collected from each subject before and at several times after each meal. The insulin, glucose, free-fatty acids, and glucagon levels in the blood were analysed.
This study showed that serum glucose and insulin responses were different for meals having high and low GI levels. There was a virtual straight line relationship between the meal GL and serum glucose and insulin response in terms of the peak levels. These differences applied for both small and large meal sizes. However the higher serum glucose response only occurred when larger meals were eaten.
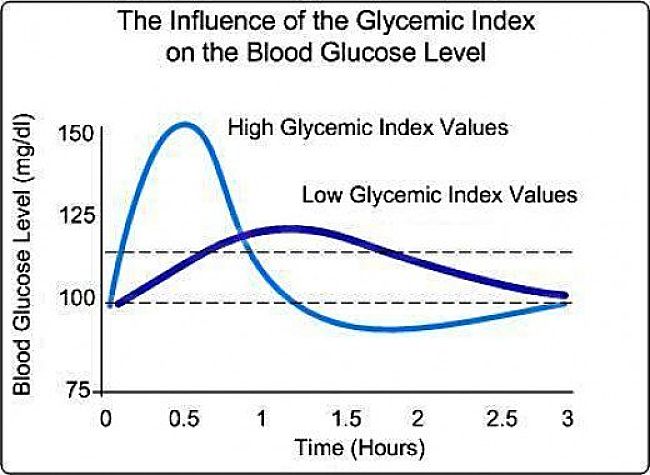
The two images below highlight the so-called ‘overshoot’ and ‘undershoot’ caused by eating foods high in sugar and corn syrup.
The results clearly demonstrate that eating sugar creates a higher and quicker peak in both blood sugar and insulin. The pronounced drop in blood sugar levels may also be significant and be signs of a sugar craving.
High GI foods have a more pronounced effect on blood glucose levels. They are more quickly digested. The sugar and carbohydrate is released into the blood in a rush and produces a pronounced high peak in blood sugar. The insulin response is similarly a very high and pronounced peak. For low GI and low GL foods the carbohydrate is released more slowly and the graph shows a flatted curve without a sharp peak and under shoot.
Are Sugar Cravings Symptoms of an Addiction for Sugar?
A recent study has examined the theory that sugar addiction may play a role in obesity and eating disorders. There was evidence that the high and fast spike and subsequent dramatic decline in blood sugar, that comes after eating highly processed carbohydrates and sugars, activates reward and addiction centers in the brain.
This suggested that avoiding refined carbohydrates, and the spikes in blood sugar they produce, might be a good way to lose weight because people would eat less and not succumb to the strong sugar cravings that are induced by the wild swings in blood sugar and the effect it has on moods and feelings. Limiting highly processed foods, sugary foods and beverages, may help people control their overeating tendencies. Perhaps in time they might lose their addiction to corn syrup and cravings for sugar.
The research suggests that eating sugar and refined carbohydrates are linked to pleasurable feelings. In one experiment, two groups of overweight and obese young men were given two separate drinks.
- One drink contained corn syrup, with a very high GI and GL
- The other one contained cornstarch, which has low GI and GL, and leads to a more gradual rise in blood sugar with a lower peak.
Zero-calorie sweeteners were used to ensure the two drinks very similar, with equal sweetness .
The men who consumed the high GI drinks showed a dramatic spike in blood sugar after consuming the drink. After only 4 hours, their blood sugar levels crashed to very low levels, and they started to feel very hungry again and craved sugar.
Brain scans of those subjects who drank the corn syrup drink showed increased activity in the region of the brain that has been linked in other studies with reward and cravings and addiction responses.
This study only looked only at obese and overweight subjects with a small sample size.
Various previous review studies have failed to show conclusively that sugar cravings are a classical addiction like nicotine.
Nevertheless sugar cravings may be have preliminary addiction properties.
Further studies are needed to clarify this.
Big Dips in Blood Sugar Levels Linked to Early Onset Hunger Pangs
Learning how to control appetite, delay its onset after meals has been shown to be a key element in weight control. The hunger pangs that occur between meals can cause many people to consume snacks between meals, which adds to their daily calorie intake.
Recently published research demonstrated that people who show big dips in blood sugar levels, about 2-4 hours after eating a meal, can start feeling hungry much sooner after eating a meal. Consequently, they may end up eating more snacks and so consuming many more calories during each day than others who experience much smaller dips.
It has long been known that blood sugar levels often fall in the first two hours after a meal, after reaching what has been referred to as the blood sugar peak. Many diet intervention strategies for weight control focus on preferences for complex low GI foods that contain fiber and take lower to digest that high carbohydrate and sugary foods. However, recent research has shown that some people showed major 'dips in sugar levels' about 2-4 hours after this initial blood sugar peak. The blood sugar levels dropped quickly below their baseline before coming back up to normal levels. The researchers referred to these people as 'big dippers', who may have a genetic predisposition to this response compared with the general population.
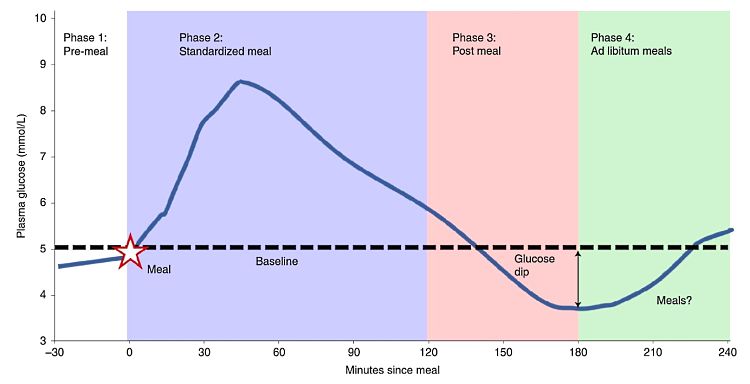
The features shown by 'Big Dippers' compared with 'Little Dippers' who showed only a small drop in blood sugar were highlighted by the study:
- Big dippers had about a 10% increase in hunger feeling at this time,
- Big dippers waited about half an hour less, on average, before their next meal meal or snack, even though they ate exactly the same meals.
- Big dippers consumed about 75 more calories in the 3-4 hours after breakfast than little dippers
- Big dippers consumed 312 extra calories over the whole day than little dippers.
- Big dippers could, through this extra calorie consumption potentially gain 20 pounds of extra weight over a year.
The study explored the links between appetite, postprandial glucose and subsequent energy intake in 1,070 participants after eating the same standardized breakfast and freely chosen meals over a 14 day period. The standard breakfasts were based on muffins, which containing the same number of calories but which had varying proportions of protein, carbohydrates, fat and fibre.
Each participant wore a stick-on continuous glucose monitor. These were used to track how their blood sugar levels varied throughout the day. A wearable device was also worn to monitor activity levels and sleep to account for calorie burn rates. The researchers also recorded the perceived levels of hunger felt by each of the subjects and their alertness using a phone app. The same app was used to record exactly when and what each subject ate during the day.
The study found that the size of sugar dips (BIG and LITTLE) in the 2-4 hours after eating had a very large impact on hunger and appetite. Even when the participants ate the same test meals, the study revealed large differences in blood sugar responses between various people. The researchers found no correlation between body weight, age, or BMI and being the BIG and LITTLE dipper groups. It appears that this was related to their genetics rather than their body shape, weight and eating habits. However, males showed slightly bigger dips than females on average for the subjects in the study. The study suggested that whether you're a BIG dipper or a LITTLE dipper depends on individual inherent differences in metabolism.
Interestingly, there were major differences in how far below normal, the blood sugar level dipped in certain individuals in response to eating the same meals on different days. There was some evidence that the size of the dip from day to day depended on the effects of snack meal choices, eating patterns and activity levels. This suggested that BIG dip subjects could choosing foods and activities which could in same ways ameliorate for their unique metabolism. This could help people learn to feel fuller for longer, have lower dips between meals and eat less overall.
The study was published in Nature Metabolism
Postprandial glycaemic dips predict appetite and energy intake in healthy individuals. Nature Metabolism, 2021; DOI: 10.1038/s42255-021-00383-x