Links Between Dietary Fat Intake in Food, Obesity and Weight Loss
There is a lot of debate about the role that dietary fat plays in obesity and heart disease and there has been criticism of advertisement campaigns targeting fatty foods for being simplistic and conveying the wrong message. Is Dietary Fat the real problem increasing the risk of obesity, heart disease and other health problems? Should this be the target of the campaigns?
The Australian Medical Association, in 2011, has approved the use of a series of frighteningly graphic television advertisements in Australia to warn people about the risks of eating fatty foods and drinking sugar laden drinks. The alarming increases in the rates and cost of obesity has triggered these extreme responses.
The proposed ads in television and newspaper would cost about $25 million and would show the effects of fat on the body’s internal organs. A similar American ad includes a warning that just one sugary soft drink a day over a year can make you up to five kilograms fatter and increase the risk of obesity, diabetes and heart disease. These proposed ads are designed to alarm the audience about the damage fat does to the body, much like the scary 'quit smoking' advertising campaigns.
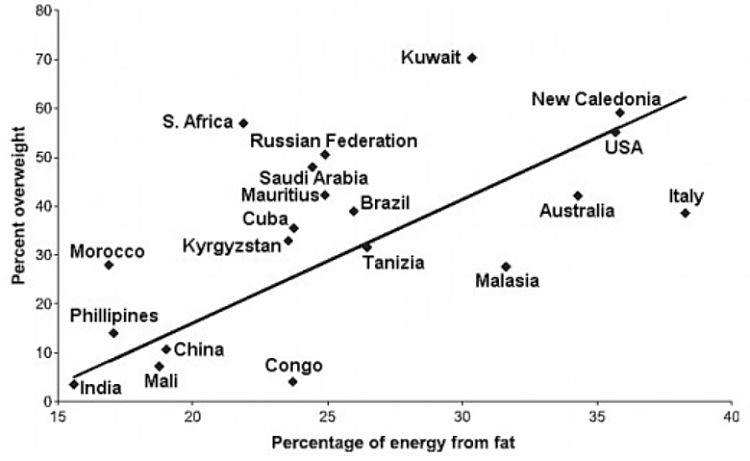
The figure below shows the association between the proportion of energy from fat with the prevalence of overweight (body mass index, BMI, of 25 kg/m2 or greater) amongst adults from 20 countries. There was a significant positive association between fat consumption and the proportion of the population who are overweight. This suggests that halting the increase in dietary fat in many countries where the diet is traditionally low in fat may be an effective strategy to prevent an increase in obesity.
Link Between Dietary Fat and Obesity - True or False?
Despite the claims and assumptions that have proliferated, other studies show that this association between fat consumption and obesity may be misleading.
The National Heart Foundation of Australia’s review of the relationship between dietary fat and cardiovascular disease (CVD) showed a link between the amount of saturated fat in the dietand cardiovascular disease risk, but found little evidence demonstrating that coronary events or death are linked to the amount of total fat in the diet.
But it has been suggested that dietary fat intake could increase the risk of CVD indirectly by causing people to become overweight and obese, as excess weight is a major risk factor for morbidity and mortality related to coronary heart disease (CHD).
They conducted a review of the relationship between dietary fat and overweight/obesity, which is summarized below:
- Dietary fat is not an independent risk factor for the development and progression of overweight and obesity (moderately good evidence for this).
- Energy balance (calories eaten and burnt) is clearly the major determinant of weight loss. A strategy of reducing dietary fat is a simplistic behavioural strategy to achieve energy restriction. However, without calorie intake restrictions, fat reduction alone is not effective for achieving weight loss in overweight and obese individuals (moderately good evidence for this).
- Dietary fat reduction alone may be effective for preventing weight gain in normal weight, overweight and obese individuals (minor evidence for this).
- It was recommended that public health nutrition strategies for the prevention of cardiovascular disease emphasise reducing saturated fatty acid intake.
The study concluded that the energy density of food may be a major determinant of energy intake, although protein intake may act independently of this.
Further research is required to determine the relative effectiveness of manipulating the dietary fibre and water content of foods on reducing the energy density of the overall diet.
Other dietary and non-dietary factors are also implicated in the development and progression of overweight and obesity. Clearly physical activity plays an important role in regulating body weight. Further research is required to determine the combined effect of dietary and physical activity strategies in weight management.
Do High Fat Diets Cause Obesity?
There is major debate about whether the percentage of dietary fat in the diet plays an important role in the increasing prevalence of overweight and obese people in the population, and in its treatment once it has developed. A reduction in fat intake reduces the gap between total energy intake and total energy expenditure and thus is an effective strategy for reducing the present epidemic of obesity worldwide.
A review of the results from 28 clinical trials that studied the effects of a reduction in the amount of energy from fat in the diet showed that a reduction of 10% in the proportion of energy from fat was associated with a reduction in weight of 16 g/d.
Studies of rats showed that diets high in fat content causes increased caloric intake and promotes weight gain. Dietary fat is calorically dense and hence higher levels of dietary fat increase the susceptibility to diet-induced obesity in growing rats by stimulating caloric intake, fat accretion, and weight gain.
Energy density appears to be a major determinant of energy intake.
The energy density of the diet is mainly determined by the dietary fat, fibre and water contents of foods.
It is possible that dietary fat may increase the energy density of the diet, facilitating excess energy intake and hence indirectly increase the risk of overweight and obesity.
However, other factors may also influence energy intake including the palatability and the physical form of food, the amount (portion size) and volume of food consumed.
There is therefore, moderate evidence suggesting that dietary fat is not an
independent risk factor for the development and progression of overweight and
obesity.
Energy balance is the major determinant of weight loss.
Other studies suggest that reducing fat in the diet may help reduce net energy intake, resulting in modest short term weight loss.
Studies comparing energy restricted diets (around 5040kJ/day) with low fat ad libitum diets (25% E or 30 - 35 g/day) suggest that they are equally effective in reducing energy intake and achieving short term (6 months) weight loss in overweight and obese individuals.
However, weight loss is not maintained in the long term due to poor dietary compliance with both diets.
A low energy dense diet may be achieved on a moderate dietary fat intake (around 35% E fat) by including plenty of vegetables in the diet.
Further research is required to determine the relative effectiveness of manipulating the dietary fat, fibre and water content of foods on reducing the energy density of the overall diet.
There is therefore substantial evidence suggesting dietary fat reduction alone, without energy restriction, will not achieve weight loss in overweight and obese individuals.
In particular, replacing dietary fat with carbohydrate will not produce the energy deficit required to achieve weight loss.
Dietary Fat and Weight Gain in Women
A Women’s Health Initiative (WHI) study seems to confirm this. The results of one study, published in the Journal of the American Medical Association, showed no benefits for a low-fat diet.
Women assigned to this eating strategy did not appear to gain protection against colorectal cancer, breast cancer, or cardiovascular disease.
And after eight years, their weights were generally the same as those of women following their usual diets.
Another WHI study looked at how the weight of a group of about 19,000 post-menopausal women was changed when they were told to follow a low-fat diet. The women were supposed to reduce their dietary fat to only 20 percent of their calories.
Most women did not reach their low goal, but they did progress from diets that averaged 38.8 percent fat (rather high) at the beginning to diets with 29.8 percent fat (which is considered a low-fat diet) at the end.
To see if fat alone affected weight, the women were told to eat more carbohydrates to replace the fat their eliminated from their diet to try to maintain their initial weight. At the beginning of the study, 74 percent of the women were overweight or obese. The results were:
- Firstly, does eating less fat for better health lead to weight gain if you eat more carbohydrates? The study found that this was not the case. You can cut back on fat without having a weight gain. However, to achieve better health benefits you should aim to greatly reduce your saturated and trans fat consumption.
- Secondly, can people lose weight by reducing fat in their diet without reducing calorie intake or changing their exercise habits (the balance of energy consumed and burnt) ? For the group of women over age 50 in this study, the answer was no.
- The conclusion is that if you reduce fat in your diet but substitute other foods to maintain the same calorie intake, you shouldn’t expect to lose weight.
Change in your energy balance almost always requires eating fewer calories.
Eating less fat, without substituting calories from other sources, is a good way of doing this.
If you currently eat few fruits, whole grains, vegetables and beans, eating more of these foods may help fill you up, and help you cut down on foods with high energy densities such as fat, processed foods and sugar.
However,simply eating more healthy food like vegetables and fruits is unlikely to cause weight loss unless you reduce portion sizes and the total amount that you eat.
Another study showed the benefits of healthy diet for older people is to increase life expectancy.
Research reported in the Journal of the American Dietetic Association compared the diets of 2,500 US adults aged 70 to 79.
The study found that individuals with a low-fat diet and plenty of fruit and vegetables reduced their risk of dying over a ten year period.
Those people who ate diets rich in cheese, ice cream and whole milk, had the highest risk of death.
The study showed that a healthy diet meant that and extra 12% of people survived over the ten year period. The volunteers were divided into 6 dietary groups, depending on the frequency with which they consumed certain foods.
The food groups were: healthy foods; fried foods and alcohol; high-fat diary products; meat, breakfast cereal; refined grains and sweets and desserts.
Researchers found that those with a high fat diet rich in dairy products had a higher death risk than those in the healthy food group.
The death risk for the "healthy foods" eaters and the "breakfast cereal" or "refined grains" eaters were not significantly different.
The most harmful food groups appeared to be the 'high fat dairy group' and 'desserts and sweets' group. These groups are both high in trans fatty acids and saturated fat, in addition to calories, contributing to obesity and high cholesterol problems.